Introduction
Provision of health services is a devolved function and county governments are expected to plan and budget for it. For the counties of Mandera, Wajir, and Garissa, devolution has been a blessing. These counties have for decades faced successive marginalization resulting in lack of access to essential services including health care services. Most of the counties had poor health indicators in maternal and infant mortalities, health financing, human resources for health (HRH), essential medicines, medical equipment, and supplies, and access as facilities are far apart with limited referral services. Devolution presented unprecedented opportunities as the power to plan, manage and make decisions around resources has moved from the centre to the sub-national level. In health, services have moved closer to the people to meet their needs in a more equitable manner.
With improved funding to the counties, service delivery indicators have tremendously improved across all the counties. Data from the Kenya Health Information Systems (KHIS) have shown that the percentage of deliveries conducted by Skilled Birth Attendants (SBA) for Garissa County increased from 43.5% to 61.9% between 2017 and 2021, while in Mandera it improved from 31.4% to 75.8% and in Wajir from 41.6% to 46.5% over the same period. At the same time, the proportion of children under one year who were fully immunized improved between 2017 to 2021 from 55.4% to 81.3% for the county of Garissa whereas in Mandera this has greatly improved from 37% to 81%.
Other notable changes in the counties include infrastructural development and increasing access to service deliveries. Public health facilities have increased at all levels in all the counties. Garissa County currently has 94 facilities, Mandera 92 and Wajir 115 public health facilities. In addition, specialized services such as CT scan, Oxygen plants, ICUs, Dialysis units, and state-of-the-art diagnostic facilities have been established. Referral and lifesaving emergency services are provided to reach the hard-to-reach communities and peripheral facilities.
Policy Issue
Counties receive funding for health care through an allocation set aside for county governments, and through grants such as the leasing of medical equipment often termed as Managed Equipment Services (MES), Free Maternity health care, National Health Insurance Fund (NHIF), compensation for user foregone fees, DANIDA grant, World Bank loan to supplement county health facilities, World Bank loan for Transforming Health System for Universal Care Project and User fees for level 4 and 5.
Despite the budgetary allocation to health, most of the counties in North Eastern did not start on the same footing as the rest of the country due to successive marginalization. As such, the financing allocated to health infrastructure and other service delivery indicators is not wholly adequate. In addition, the donor landscape and financing from development partners have been dwindling and are likely to be phased out completely.
Current and Past Interventions
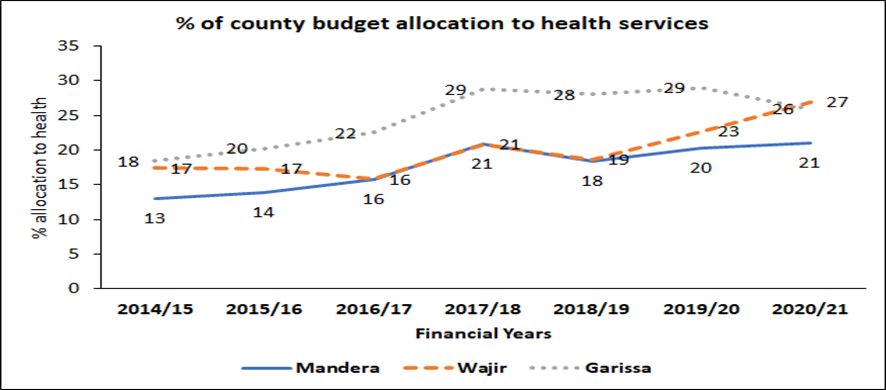
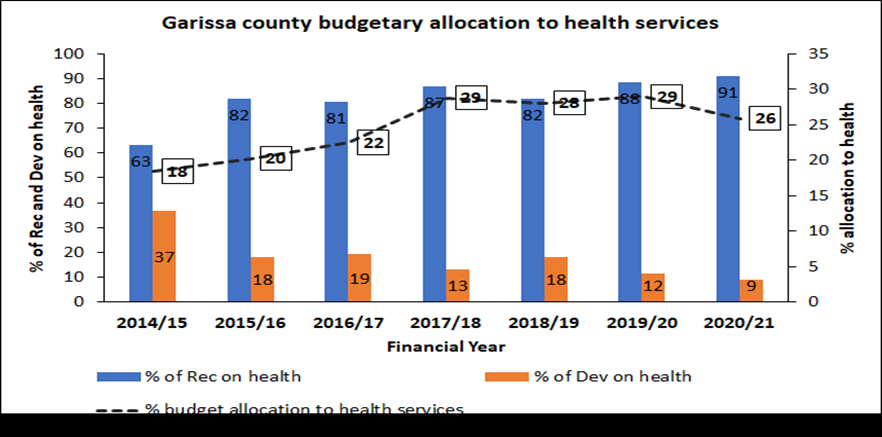
With devolution, most of the counties are now able to allocate more resources to delivery of health services. Between the financial years 2014/15 and 2020/21, Mandera, Wajir and Garissa counties have allocated an average of 18%, 20% and 25%, respectively, to the health sector as a share of total county budget allocation. The county of Mandera had the highest approved county budgetary allocation of Ksh 87.09 billion while Garissa county had allocated Ksh 62.56 billion over the same period. The figure below indicates a progressive trend in budgetary allocation to county health services. Garissa county had made the highest budgetary allocation from 18% in 2014/15 to 29% in 2019/20, with a slight drop to 27% in 2020/21. Mandera county has moved from 13% in 2014/15 to a high of 21% in 2020/21. Despite slight fluctuations, Wajir county made steady progress from 17% to 26% between 2014 and 2021.
The Managed Equipment Services (MES) had the overall objective of scaling up health infrastructure for specialized medical care such as dialysis, basic and advanced surgery, emergency, critical care, and imaging services. These counties received and installed renal dialysis machines, sterilization equipment, and CT-scans. However, the design of the MES project was never informed by the needs of these counties as “one size fits all” in the supply of the medical equipment was done, yet counties at the onset of devolution did not set off at the same footing. This has led to under-utilization of delivered medical equipment due to lack of trained personnel to operate the machines, and inadequate supporting infrastructure such as space and power. The annual payment for the medical equipment by counties has also been fluctuating over the years from Ksh 95 million in 2015/16 to Ksh 200 million in 2018/19.
Universal Health Care (UHC) meant that all individuals and communities should receive health care services without suffering financial hardships, including essential quality health care services from health promotion to prevention, treatment, and rehabilitative services across their life course. In all three counties, UHC has been rolled out and indigents were registered and provided with NHIF cards that can be used at the facilities where they are registered. However, the number of households registered in each of the three counties were few. For instance, Mandera county with more than 125,000 households registered only 22,000 principal indigents, meaning that many of the residents still do out-of-pockets in financing health care services. In addition, the services that they currently received through NHIF at the health facilities are limited in scope.
Currently, the conditional grants to level 5 hospitals are only for the former provisional and national referral hospitals. Therefore, Garissa County Referral Hospital continues to receive grants targeting medical and surgical subspecialties, intercounty referral services, and medical training. The rest of the other counties lack such arrangements despite having level 5 health facilities.
The counties responded to the COVID-19 pandemic through increased allocation of funds in the 2019/20 and 2020/21. For instance, Mandera county allocated Ksh 180 million in 2019/20, in addition to Ksh 391.32 million grants from the National Government, Ksh 11.31 million as DANIDA for COVID-19 in the 2019/20, with the total fund available for COVID-19-related expenditure amounting to Ksh 614.47 million. Wajir county also allocated Ksh 112.79 million to cater for COVID-19-related expenditure in 2020/21, while Garissa was allocated Ksh 118.52 million in 2020/21 (Office of the Controller of Budget 2020/21).
Other conditional grants through development partners such as World Bank (Transforming Health Care for Universal Care Projects) support the improvement of Reproductive, Maternal, Neonatal, Child, and Adolescent Health (RMNCAH) indicators. DANIDA grants for user forgone fees to level 2 and 3 public health facilities mainly for operation and maintenance are likely to come to an end in all these counties by 2025.
Gaps and Emerging Issues
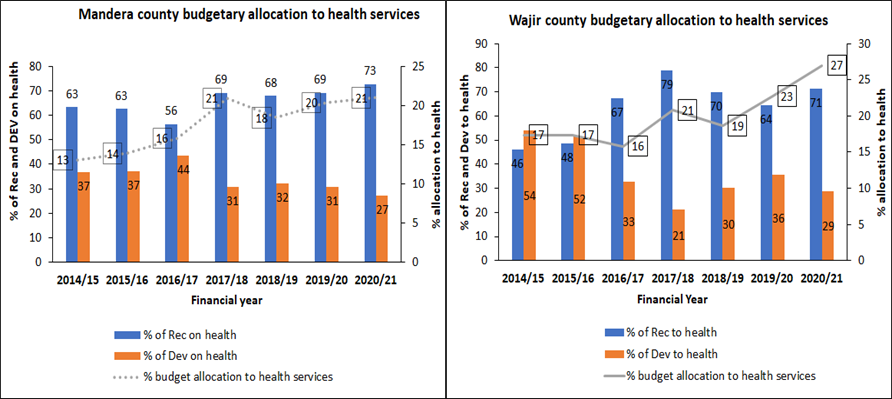
Despite the huge allocations to the health sector, analysis of the three counties’ budget indicates that much of the funds are allocated to recurrent expenditure. For example, Garissa County had the highest allocation of an average of 82% to recurrent with only 18% left for development, which is below the requirement of the PFM Act of at least 30% of the budget allocated to development. Most of the recurrent expenditures are on personal emoluments, leaving little for the provision of service delivery including preventive and promotive health services.
In addition, development partners who mainly support health systems strengthening are dwindling and have become unpredictable. The main partners in financing primary health facilities such as DANIDA are likely to wean-off counties by the year 2025, and counties are expected to finance primary health facilities at 100%. In addition, the World Bank loan of transforming health systems for universal care project, which aims to improve the use and quality of primary health care services with a focus on reproductive, maternal, newborn, child, and adolescent health services is also expected to end by the year 2023. If this is not abated, it will reverse back the gains made in improvement of the health service delivery indicators, especially at the primary health facilities.
While significant progress has been made in recruitment of health care staff in these counties, the required mix of cadres are below the norms and standards for human resource for health, which requires significant financial resources.
Way Forward
From the foregoing, counties in collaboration with the National Government and development partners should address health care financing through:
- Increased budgetary allocation to health care service delivery.
- Planning, budgeting, enrolling more indigents on NHIF, and increasing the scope of the services that they can seek, including specialized care, to achieve Universal Health Coverage by 2030.
- Prioritization of development projects such as oncology centres for provision of specialized cancer care service as none of the counties have these services.
- Resource mobilization from health development partners in addressing key gaps in health care financing.
- Planning and budgeting gradually for primary health care facilities to close the gap that is likely to be left by DANIDA support.
- Enhancement of human capital development through training of more specialized cadres on use of specialized medical equipment.
- Investment on preventive and promotive health care services.
Authors: Hassan Ali, Young Professional, Social Sector Department
Martha Naikumi, Young Professional, IESD Department